- Home
- Common Shoulder Problems
- Labrum Tears
- Bankart Lesion
Bankart Lesion
Written By: Chloe Wilson BSc (Hons) Physiotherapy
Reviewed By: SPE Medical Review Board
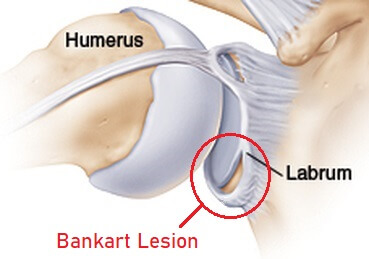
A Bankart lesion, aka glenoid labrum tear, is where there is damage to the special layer of cartilage lining the shoulder joint.
A bankart tear usually occurs when the shoulder dislocates forwards and most commonly affects young athletes.
Labrum tears makes the shoulder more prone to instability and there is a high risk of further shoulder dislocation without appropriate treatment.
Bankart lesions are named after English Orthopedic Surgeon Arthur Sydney Blundell Bankart, 1879-1951, who first described the injury and the surgical repair process.
Here we will look at the common causes, associated injuries, symptoms and treatment options, both surgical and non surgical, for a Bankart lesion labrum tear.
What Is A Bankart Lesion?
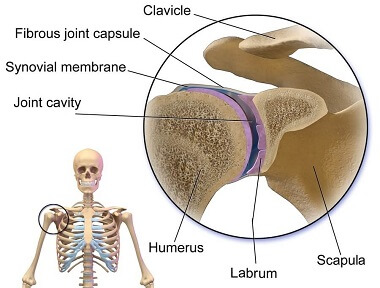
To fully understand Bankart lesions, we need to first understand the structure of the shoulder. The shoulder joint, aka glenohumeral joint, is a ball and socket joint, similar to the hip joint. It is made up of the:
- Ball: the top of the arm bone (head of the humerus)
- Socket: front part of the shoulder blade (glenoid fossa)
The shoulder socket is very shallow, much shallower than the hip socket. This is because the shoulder needs to be able to move in multiple directions through a huge range of movement.
Imagine a golf ball sitting on top of a golf tee, not very stable. So around the rim of the socket is a special band of cartilage known as the glenoid labrum. This labrum is made of fibrocartilaginous material and works to deepen the socket to improve the connection of the joint and improve shoulder stability without restricting mobility.
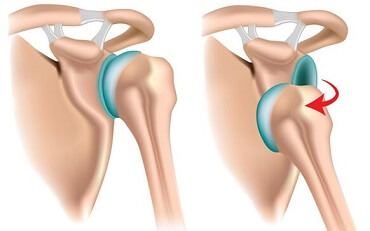
A Bankart lesion is when there is damage to the lower portion of the glenoid labrum, causing it to tear away from the bony socket.
What Causes A Bankart Lesion?
Bankart lesions are typically caused by an anterior dislocation of the shoulder, where the head of the humerus is forced forwards and pops out of the glenoid socket. As the bone is forced forwards, it can damage the labrum, causing it to tear.
Approximately 95% of Bankart lesions are due to anterior shoulder dislocations, typically caused by:
1. Trauma
Bankart lesions are often caused by a fall onto an outstretched arm, particularly if the arm is:
- Abducted: out to the side
- Externally Rotated: turned outwards away from the body
- Extended: back behind the body
Falls are the most common cause of anterior shoulder dislocations in older patients and thus Bankart lesions. Road traffic accidents (RTA’s) are another traumatic cause of shoulder dislocations.
2. Sports Injuries
Another common cause of anterior shoulder dislocations and bankart tears are contact injuries e.g. football or rugby tackles, particularly when the arm is above the head and the elbow is pushed backwards. Repetitive arm movements above the head e.g. throwing or overhead racket sports such as tennis are another common cause.
Sporting injuries are the most common cause of a glenoid labrum tear in younger patients.
Associated Injuries
When the shoulder dislocates anteriorly, other structures may also be damaged, alongside a Bankart lesion such as:
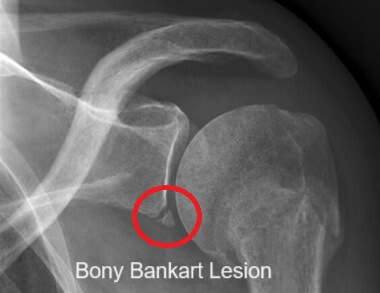
- Bony Bankart: fracture in the lower front part of the glenoid cavity
- Hill-Sachs Lesion: compression fracture on the posterolateral (outer back) part of the humeral head
- Proximal Humeral Fracture: break anywhere in the humeral head (the ball)
The joint capsule, a special sac that sounds the glenohumeral joint, may also be damaged, as may be the surrounding ligaments, most commonly the inferior glenohumeral ligament. Fluid may also collect around the labrum tear forming a shoulder cyst.
These all increase the risk of further shoulder instability which makes the shoulder more prone to further injury.
Symptoms Of Glenoid Labrum Tear
Common symptoms of a Bankart lesion include:
- Recurrent Dislocations: Repeated episodes of shoulder dislocation are common with a Bankart lesion, particularly in younger patients, affecting up to 80% of people under the age of 30. This frequency reduces with age to around 30% by the age of 80
- A Feeling of Instability: The shoulder may feel weak and as if it is going to dislocate again, with actions such as throwing. A common complaint is “I just don’t trust my shoulder anymore”
- Shoulder Pain: People with a glenoid labrum tear often complain of an aching pain which tends to be diffuse rather than in one spot
- Catching/Locking Sensations: Strange sensations often occur when moving the arm with a labrum tear and you may notice shoulder clicking
- Swelling: there may be a pocket of swelling where excess fluid drains from the tear forming a paralabral cyst
Bankart Lesion Treatment
There are two treatment options for Bankart lesions, surgical and non-surgical. The right treatment will depend on factors such as age, activity levels and levels of instability.
1. Surgical Treatment
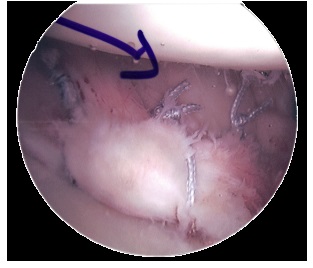
Bankart repair surgery tends to be the treatment of choice for younger patients with a Bankart lesion, especially those who play sports, as there is a high risk of the shoulder dislocating again. This is because the glenoid labrum tear often fails to heal properly, so doesn’t provide the extra depth to the socket that is needed, reducing the stability and increasing the risk of further dislocation.
A Bankart lesion repair is usually carried out arthroscopically (hey hole surgery) under general anaesthetic. The labral tear surgery aims to repair and tighten overstretched and damaged ligaments, joint capsule and cartilage, and will also remove any cysts that have formed.
Suture anchors are placed in the bone and the torn glenoid labrum is reattached to the glenoid fossa. You can usually go home the same day, or the following day after a Bankart repair.
A sling will need to be worn (including when you sleep) to protect the shoulder for the first few weeks and allow it to heal in the correct position. Physical therapy will be started almost immediately to regain strength, stability and movement. You will be given a rehab programme to follow, progressing to more challenging exercises over time. It usually takes around 4-6 months to recover completely from a Bankart repair and be able to return to contact sports.
Bankart shoulder repair surgery has an approximately 85-90% success rate, with most people returning to their pre-injury activity levels. Outcome tends to be slightly better when surgery is carried out soon after the initial labrum tear, rather than further down the line.
2. Non-Surgical Treatment

For older patients, or those who are less active, non-surgical treatment is recommended for a Bankart lesion.
The arm is immobilized in a sling for a few weeks, usually with the arm resting across the front of the body in internal rotation (turned inwards) and a small pillow under the armpit to hold the arm slightly away from the body.
This is then followed by intensive physical therapy to regain the strength, stability and mobility of the shoulder with a combination of:
- Rotator Cuff Strengthening Exercises: to improve shoulder strength
- Scapular Stabilisation Exercises: to improve shoulder stability
- Shoulder Stretches: to improve shoulder mobility
One of the problems with this treatment method is that in this rest position, the glenoid labrum tends to heal in slightly the wrong place, so the socket depth is reduced, making the shoulder more prone to recurrent dislocations.
Except for young athletes, the advice is often to try non-surgical therapy first with a bankart lesion. If the shoulder does re-dislocate, then bankart repair surgery would be advised.
What Else Can Help?
A Bankart lesion is just one possible cause of shoulder pain and instability. Shoulder labrum tears can also occur in other parts of the glenoid labrum. Damage to the upper part of the glenoid labrum is known as a SLAP tear and causes pain and instability with overhead movements.
Other common causes of upper arm pain include:
You can find out more about other causes in the Common Shoulder Problems section. If you don't think a Bankart lesion sounds quite like your problem, check out the shoulder pain diagnosis section for help working out what is going on.
Related Articles
Shoulder Problems
January 29th, 2026
Shoulder Diagnosis
February 25th, 2026
Rehab Exercises
May 21, 2024
Page Last Updated: January 29th, 2026
Next Review Due: January 29th, 2028