- Home
- Common Shoulder Problems
- Bursitis
- Scapulothoracic Bursitis
Scapulothoracic Bursitis
Written By: Chloe Wilson BSc (Hons) Physiotherapy
Reviewed By: SPE Medical Review Board
Scapulothoracic bursitis, also known as “snapping scapula syndrome”, develops when there is a problem with how the shoulder blade moves over the rib cage.
Inflammation of one of the two bursae that sit between the scapula bone and the subscapularis muscle affects how the shoulder blade moves causing friction, weakness and pain.
Scapulothoracic bursitis causes a constant, dull ache around the shoulder blade and sufferers often complain of a “snapping” or “grinding” sensation when they move their arm.
Scapulothoracuc bursitis is a rare condition, most commonly affecting young athletes who do lots of overhead action such as throwing or swimming. However previous shoulder problems such as ligament tears and arthritis also increase the risk of developing scapulothoracic bursitis.
Here we will look at the common causes, symptoms, diagnosis and treatment options for snapping scapula syndrome.
What Is Scapulothoracic Bursitis?
All around our bodies, there are numerous bursa. These are small fluid filled sacs that act as cushions, providing lubrication between tendons and bones, allowing smooth, friction-free movement.
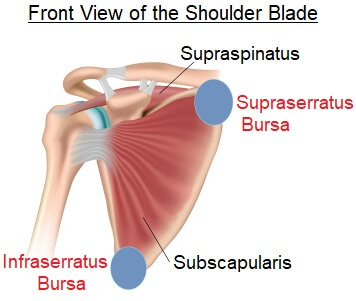
The subscapularis muscle is a large muscle that sits between the shoulder blade and the rib cage.
There are two bursa, known as infraserratus and supraserratus, that sit between the muscle and the bone allowing the shoulder blade to glide over the chest wall freely as the arm moves. One is located at the top of the shoulder blade, the other at the bottom.
A large proportion of shoulder movement comes from the shoulder blade so it is really important it can move smoothly and freely. Weakness in the shoulder blade muscles leads to subtle changes in the angle of the shoulder blade which affects how it moves. It may then start to rub against the rib cage which leads to inflammation of the subscapular bursa and surrounding tissues.
Causes of Snapping Scapula Syndrome
Scapulothoracic bursitis is generally caused by problems with the bones or soft tissues of the rib cage and shoulder blade.
Common causes of snapping scapula syndrome include:
- Overuse: Repetitive friction from overhead activities such as throwing, weight lifting, tennis or swimming places irritate the bursa causing inflammation
- Weakness: muscle weakness means there is less bulk between the ribcage and shoulder blade so they sit closer to each other. The bones can end up rubbing against each other leading to inflammation
- Posture: Sustained, kyphosed (forward flexed) posture can lead to weakness of the subscapularis muscle and shift the position of the shoulder blade slightly which makes the bursa prone to friction
- Trauma: Injury to the surrounding area from e.g. a fall
- Medical Conditions: inflammatory conditions such as rheumatoid arthritis increase the risk of developing scapulothoracic bursitis
- Poor Scapular Mobility: Anything that affects how the shoulder blade moves can increase friction and lead to scapulothoracic bursitis. It may be muscle weakness, a nerve problem or another shoulder problem such as a frozen shoulder
- Bony Abnormality: If the bones are not smooth, there will be more friction on the surrounding soft tissues. There may be extra bone growth on the scapula such as a Luschka tubercle (hooked shape prominence on the inner top corner of the scapula), a bone tumour such as an osteochondroma or as a result of a previous injury such as a rib fracture
Scapulothoracic Bursitis Symptoms
The most common symptoms of scapulothoracic bursitis are:
- Snapping: The most prominent feature of snapping scapula syndrome is a snapping/grating/grinding noise or sensation at the shoulder blade during arm movements
- Pain: Usually described as a constant, dull, aching pain around the shoulder blade and ribcage. The pain tends to get worse with arm movements, particularly when reaching above your head or when doing press ups
- Lump: There may be a small lump that you can feel on the shoulder blade if there is excess bone growth
Your doctor will usually be able diagnose scapulothoracic bursitis by talking to you about your symptoms and observing your shoulder and scapula movements. In some cases they may do an x-ray, MRI or CT scan.
Snapping Scapula Treatment
Most cases of scapulothoracic bursitis can be treated without the need for surgery, but in a few stubborn cases, surgery may be necessary.
#CommissionsEarned from Amazon on qualifying purchases
Non-Surgical Treatment
Non-surgical treatment for scapulothoracic bursitis involves:
- Rest: Avoiding aggravating activities and movements helps reduce the friction and pressure on the bursa. However, it is important to keep the shoulder moving within pain limits to prevent it from stiffening up
- Medication: Non-steroidal anti-inflammatory medication such as ibuprofen/Advil can help to reduce pain and inflammation. Always check with your doctor before taking any medication

- Physical Therapy: Working on a rehab programme with a physical therapist will help to restore normal shoulder blade movement. This will include strengthening exercises for the muscles that move and control the shoulder blade and upper back stretches.
If there are other problems affecting how the shoulder joint moves, they will be addressed too which may include stretches and further strengthening exercises for the rotator cuff muscles. You will need to work on your home exercise program daily for a number of weeks.
- Improve Posture: improving your posture can really help both treat scapulothoracic bursitis but also stop it from coming back. This is particularly important if you spend long periods sitting in front of a computer or on the phone. There are some really simple things you can do to improve posture that can make a big difference such as wearing a simple posture support
- Steroid Injection: In some cases your doctor may offer you a steroid injection to help to reduce the pain and inflammation from scapulothoracic bursitis. A mixture or cortisone and local anaesthetic is injected in to the bursa. It usually gives good relief of symptoms and it also confirms diagnosis, as an improvement of symptoms confirms that the symptoms were coming from the bursa.
Injections should not be used in isolation though. Whilst they help to reduce the pain and inflammation, if the underlying cause of scapulothoracic bursitis is not addresses, symptoms will most likely return. You can find out more about how injections work and the potential risks on our sister site - Cold Or Heat Packs: Many people find that using either a cold pack or a heat pack over the shoulder blade helps to reduce their pain. You can use a simple method e.g. a bag of frozen peas wrapped in a towel or a hot water bottle with a fluffy cover, or a specially designed shoulder wrap.
Heat or ice should only be used for 10 minutes at a time and you should wait 2 hours between applications.
Surgical Treatment
If symptoms of scapulothoracic bursitis have failed to settle with non-operative treatment you may be advised to have surgery.
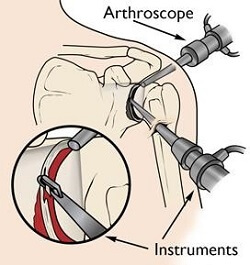
This is usually performed arthroscopically (key-hole surgery) as a day case, so you can go home the same day. Surgery for scapulothoracic bursitis may involve one or both of the following:
- Bursectomy: Removal of the inflamed bursa and any surrounding scar tissues
- Partial Scapular Resection: Removal of any bony prominences found on the scapula that may be rubbing on the rib cage. This tends to be the upper border of the inner side of the shoulder blade, known as the superior angle of the scapula.
An additional small open incision may be performed when performing the excision depending on your surgeons preferred technique
Recovering From Surgery
Following scapulothoracic bursitis surgery your arm will most likely be immobilised in a sling for up to four weeks to allow the shoulder to heal. A physical therapist will work on a graded rehab programme with you starting with passive exercises (where the weight of the arm is supported) to keep the shoulder moving well.
After approximately four weeks you will progress to more active range of motion exercises and should be able to do most of your normal daily activities. Strengthening and resistance exercises are usually introduced after around twelve weeks. Most people make an excellent recovery from scapulothoracic bursitis surgery and return to all their usual activities within four months.
What Else Can Help?
Bursitis can develop in any one of the many shoulder bursa, such as subacromial bursitis - we look at the different types in the shoulder bursitis section.
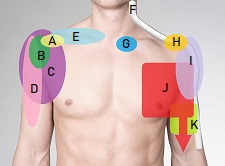
There are a number of other things that cause pain around the scapula - have a look at the shoulder blade pain section to find out what else it could be or have a look at our shoulder pain diagnosis charts.
You may also be interested in the following articles:
- Front Shoulder Pain
- Shoulder Lumps & Bumps
- Resistance Band Shoulder Exercises
- Burning Shoulder Pain
- Shoulder & Arm Pain
Related Articles
Shoulder Problems
January 29th, 2026
Shoulder Diagnosis
February 25th, 2026
Rehab Exercises
May 21, 2024
Page Last Updated: November 5th, 2024
Next Review Due: November 5th, 2026