- Home
- Shoulder Pain Causes
- Shoulder Fractures
- Humeral Shaft Fracture
Humerus Fracture
Written By: Chloe Wilson BSc (Hons) Physiotherapy
Reviewed By: SPE Medical Review Board
A humerus fracture is the medical term for a break in the bone of the upper arm. The humerus is the long bone that sits between the shoulder and the elbow.
Humeral fractures can be classified into three types, depending on which part of the bone is broken:
- Proximal Humerus Fractures: when the bone is broken at or near the top, by the shoulder.
- Mid-Shaft Humeral Fractures: a break somewhere in the middle section of the bone.
- Distal Humerus Fractures: where the bone is broken near the elbow
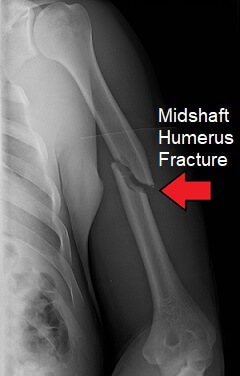
Mid-Shaft Humeral Fractures
Fractures in the long, middle section of the upper arm – mid-shaft humeral fractures, are also known as "humeral shaft fractures" or "diaphyseal humerus fractures".
Approximately 3-5% of all broken bones are midshaft humeral fractures. They tend to affect young males (20-30’s) who have experienced a high-energy injury and elderly females (60-70’s) with low-energy injuries.
Here we will look at the common causes of midshaft humerus fractures, the different types and how they are classified, classic symptoms, how they are diagnosed, the different treatment options both surgical and non-surgical, the recovery process and possible complications.
You can find out more about the other types in the shoulder fracture section.
Humeral Shaft Anatomy
The shaft of humerus can be divided into thirds, the proximal (upper third), middle (mid third) and distal (lower third).
The mid-shaft region of the humerus is the long, thin part of the bone. The top part is cylindrical in shape and as it runs down towards the elbow it becomes narrower and more prism shaped. The back surface of the shaft of humerus is larger than the front.
Causes of Mid-Shaft Humerus Fractures
Common causes of mid-shaft humerus fractures include:
- Falls: the most common cause of a mid-shaft humeral fracture, particularly in the elderly, is a simple fall. Occasionally it may be caused by falling onto an outstretched hand when the arm is abducted – out to the side
- Direct Blow: high energy force to the upper arm often causes a transverse fracture
- Torsion: Forceful twisting of the upper arm can lead to a spiral fracture. Long, spiral humeral fractures in children should be carefully examined as they may indicate abuse
- Bone Disease: Metastatic breast cancer can cause spontaneous fractures here
Classification of Humerus Fractures
Midshaft humeral fractures can be classified into different types by:
- Location: which part of the bone is broken
- Fracture Pattern: the direction of the break
- Degree Of Displacement: the alignment of the broken pieces
- Soft Tissue Damage: whether the broken pieces have punctured through
- Pathological Fractures: where the break is due to underlying bone disease
1. Location
Humerus fractures can be classified by where the break is in the bone:
- Proximal Third: 30% of humeral fractures occur in the top third region
- Middle Third: 60% of mid-shaft humerus fractures occur in the middle portion
- Distal Third: 10% of humeral shaft fractures occur in the lower third near the elbow
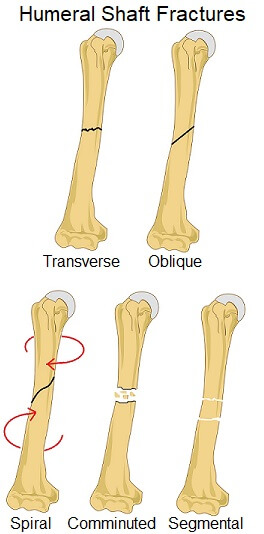
2. Fracture Pattern
Humerus fractures can also be classified by the direction of the break in the bone:
- Transverse Fracture: Where the line of the fracture runs perpendicular to the bone shaft i.e. horizontally in the humerus
- Oblique Fracture: where the fracture line is angled
- Spiral Fracture: where there is a spiral-shaped fracture line usually due to twisting of the bone
- Comminuted Fracture: where the bone breaks into several pieces
- Segmental Fracture: Where there are at least two fracture lines that together isolate a section of bone
3. Degree of Displacement
A displaced humerus fracture is where the bone fragments of the shaft do not line up normally. A non-displaced fracture is where normal alignment is maintained despite the fracture line.
4. Soft Tissue Damage
Humerus fractures are also classified by where the broken bone is visible:
- Open Fractures: This is where the skin over the fracture has been broken, typically by the broken bone puncturing through the skin from the inside, but it could also be from a blow to the shoulder cutting through the skin and muscle. Around 2-10% of humeral shaft fractures are open.
- Closed Fractures: This is where the skin remains unbroken - the opposite of an open fracture.
5. Pathological Fracture
Pathological humerus fractures are where the bone has broken due to a disease that has weakened the bone such as metastases. With pathological fractures, there may not have been a specific incident that caused the injury, the mid-shaft humerus fracture may have occurred spontaneously.
Symptoms of Humerus Fractures
The most common symptoms associated with a mid-shaft humerus fracture are:
- Upper Arm Pain: There is usually severe, ongoing pain associated with a humerus fracture
- Restricted Arm Movement: Shoulder and arm movement tends to be extremely painful so people with a mid-shaft humerus fracture are often unwilling to move their arm. There is often weakness throughout the whole arm including the wrist and hand
- Swelling & Bruising: There will be significant swelling and bruising in the upper arm which may extend all the way down to the hand. The swelling normally comes on fairly rapidly due to soft tissue damage and bleeding in the surrounding area
- Crepitus: If the pieces of broken bone rub against each other when you move your arm you may notice a grating or grinding sensation
- Deformity: If the humerus fracture is displaced, there may be an obvious deformity of the upper arm e.g. the arm may appear shorter than normal if the bone at the fracture site has overlapped
- Bleeding: If it is an open fracture where the bone has pierced through the skin, there will be bleeding
- Altered Sensation: If there is nerve damage associated with the humerus fracture, then there will be altered sensation such as pins and needles or numbness below the fracture site. Normal movement at the wrist and hand may also be affected. Radial nerve damage is common with humeral shaft fractures
Diagnosing Humeral Shaft Fractures
If you doctor suspects a mid-shaft humerus fracture you will be sent for shoulder and arm x-rays. X-rays will be taken in different directions, usually from front to back (AP) and from the side (lateral). Both the shoulder and elbow joints should be evaluated for any damage.
X-rays help the doctor to see where the fracture is, what type of humerus fracture it is, any associated damage and the severity of the injury so that they can plan the best course of treatment.
#CommissionsEarned from Amazon on qualifying purchases
Treatment For Humerus Fractures
Treatment for humerus fractures will vary slightly depending on the location and severity of the fracture, but in most cases, surgery is not required. Approximately 90% of humeral shaft fractures unite (heal) without the need for surgery.
Mid-shaft humerus fractures may be treated with:
1. Immobilisation
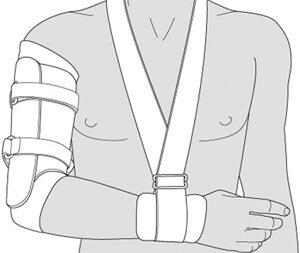
For the first few weeks after a humerus fracture, a sling or splint is worn to hold the fracture still and to allow the swelling and pain to subside. The fracture needs to be immobilised to allow time for the bones to knit back together and heal.
Humeral shaft fractures are normally treated with a "coaptation splint" that extends from the shoulder to the forearm, holding the elbow in 90 degrees flexion.
You may be given a collar and cuff sling to support the arm. It is really important to let the arm hang by your side without any support through the elbow as this allows gravity to help realign the fracture. If there is any pressure through the elbow it pushes the bones together resulting in them healing in the wrong position.
After two to three weeks the coaptation splint is switched for a functional Sarmiento Brace, a cylindrical brace that fits around the upper arm holding the humerus in place. It leaves the shoulder and elbow free to move which helps prevent stiffness.
2. Medication
Medication to relieve pain and inflammation will be prescribed following a humerus fracture. If it was an open fracture you will also be given antibiotics to help reduce the risk of infection.
3. Arm Exercises
A physical therapist will work through a rehabilitation programme with you following a midshaft humeral fracture. Exercises for the elbow, wrist and hand should be started as soon as possible to prevent stiffness and weakness from developing and it is usually fine to take your arm out of your sling to do these.
Rehab exercises following humerus fractures consist of:
- Shoulder Mobility Exercises: Once the fracture has started to unite, you can start doing some gentle exercises to get the shoulder moving. These usually start with pendulum exercises where you use gravity to move the arm, and active assisted exercises where you use your good arm to support and move the broken arm
- Strengthening Exercises: After a few weeks you will be able to start a progressive program of strengthening exercises including rotator cuff strengthening and scapular stabilization exercises. You will also be able to move on to more advanced range of motion exercises.
It is important to stick with the rehab programme and to do your exercises every day until you have regained full strength, flexibility and movement at the shoulder, elbow and hand. If you stop too soon, or only do your exercises sporadically you are likely to have ongoing limitations in the mobility, strength and function of your arm and could develop secondary problems such as a frozen shoulder.
4. Surgery
Around 10% of humeral shaft fractures will require surgical treatment. If the bone fragments are displaced, then the fragments will need to be realigned and held in place. This process is known as an Open Reduction Internal Fixation (ORIF). Usually the humerus fracture is secured with either:
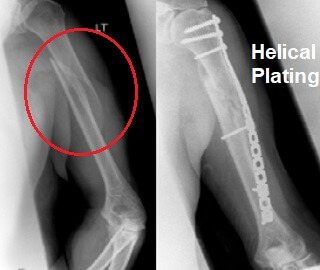
Metal Plates
Humeral shaft fractures that require surgery are usually treated with a large metal plate held in place by screws.
Pros: Highest success rate for surgical treatment of humerus fractures
Cons: Higher risk of nerve damage and non-union than non-surgical treatment
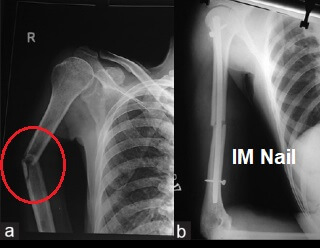
Rods
In some cases a humerus fracture will treated surgically with an intramedullary rod/nail. This is when a long metal rod is placed down the middle of the bone. IM nails can be used to stabilise a humerus fracture that is between 2cm below the surgical neck and 3 cm above the elbow.
Pros: Less invasive and less chance of nerve damage.
Cons: Lower healing rate and higher rate of non-union
Metalware is designed to hold the bones together while they heal – full union should still be achieved. Metal implants are not meant to be a long term solution and if the bones fail to unite, then there is a high chance that the metalware will at some point fail and further surgery may be required
Indications For Surgery
The usual indications for treating a mid-shaft humerus fracture surgically are:
- Fracture Can’t Be Reduced: In some cases, it may be difficult to realign the bones, or maintain the realigned position. This is usually due to associated soft tissue injuries, head injuries or patient obesity
- Open Fractures: If the bone has shifted enough to puncture the skin it is unlikely that the bone will realign without surgery
- Segmental Fractures: If the fracture has caused a fragment of bone to break off, it will often need to be secured surgically
- Multiple Fractures: If the humerus has broken into 4 or more pieces, both the left and right upper arms are broken, or there is a break in one of the forearm bones on the same side then surgery is usually necessary
- Vascular Damage: If there is significant vascular damage then surgery will be advised
- Nerve Damage: If the brachial plexus has been damaged then surgery is usually necessary. If the radial nerve has been damaged, it does not usually require surgical intervention unless there are associated injuries – the radial nerve damage will most likely heal within 3-4 months without the need for surgery
- Non-Union: If after a few weeks the humeral shaft fracture has failed to heal and the bones haven’t united then surgery may be necessary to stabilise the bone
- Skin or Soft Tissue Damage: If the skin or soft tissues of the upper arm have been damaged to the extent that it is not possible to wear a splint, e.g. severe burns, then surgery may be required
Recovery Process
Over 90% of humerus fractures treated non-operatively will unite and are usually fully healed (complete union) within 8-12 weeks. Older patients may not regain full shoulder movement, but they usually regain enough functional range for their day to day activities.
Complications are more common with complex fractures and those requiring surgery.
Mid-shaft fractures may heal with slight angulation i.e. not completely straight, but this doesn’t usually cause any functional issues as the shoulder and elbow accommodate.
Complications of Midshaft Fractures
There are a number of common complications with mid-shaft humeral fractures:
- Nerve Damage: There is often associated damage to the surrounding nerves with midshaft humerus fractures. The most commonly damaged nerve is the radial nerve, as the nerve wraps around the back of the humerus, with between 8-15% of midshaft fractures resulting in radial nerve damage. Injury to the radial nerve usually occurs at the time of injury, but can also occur when the fracture is reduced so great care should be taken when realigning the bones
- Blood Vessel Damage: There may be damage to the brachial artery
- Frozen Shoulder: This is when the capsule of the shoulder joint becomes inflamed and thickened typically due to lack of shoulder movement after a shoulder fracture LEARN MORE >
- Myositis Ossificans: This is where calcification develops in the surrounding muscles. Myositis ossificans is usually caused by returning to activities too quickly after a midshaft humerus fracture
- Fracture Angulation: Often the bone heals at a slight angle but it rarely has any function impact and is usually not visibly noticeable
- Mal-Union or Non-Union: Mal-union is when the bone fragments unite significantly out of normal alignment. Non-union is where the bone fragments fail to unite back together – this is rare with a midshaft humerus fracture occurring in only 4% of cases and tends to occur with a proximal third midshaft fracture or spiral humerus fracture.
What Else Can Help?
The best way to ensure you make a full recovery from a midshaft humeral fracture, whether it is treated surgically or not, is to follow your exercise rehab programme.
Starting exercises as soon as you can tolerate them and continuing them regularly, at least twice a day, over the next few months is the best way to regain full strength, flexibility and mobility. It can get frustrating but do persevere.
You will find a whole range of suitable exercises in the shoulder exercises section including progressive plans for mobility exercises and strengthening exercises for after humerus fractures.
You can also find out more about the different types of shoulder fractures, how the present and how to treat them in the shoulder fractures overview. If you injury is at the top part of the upper arm, visit the proximal humerus fracture section.
There are lots of other possible causes of shoulder pain. If a humerus fracture isn't sounding like your problem, check out the shoulder pain diagnosis guide.
Related Articles
Page Last Updated: November 5th, 2024
Next Review Due: November 5th, 2026